Is VA Unemployability the Same as 100% Disability? Key Differences Explained

VA Unemployability and 100% Disability: Key Differences Explained Understanding VA disability ratings can be complex, especially when comparing “unemployability” and “100% disability.” At first glance, these terms might seem similar because both result in substantial benefits, but their qualifications and implications differ. For instance, a veteran rated as 100% disabled meets specific medical criteria for […]
When Do VA Ratings Become Permanent? A Comprehensive Guide

When Do VA Ratings Become Permanent? A Comprehensive Guide For many veterans, achieving a permanent VA disability rating is a milestone that brings financial stability, peace of mind, and security in their benefits. The Department of Veterans Affairs (VA) assigns these ratings based on the severity of service-connected disabilities, with ratings ranging from 0% to […]
The Role of Medical Evidence in Mass Tort and Class Action Lawsuits

Differences Between Mass Tort and Class Action Lawsuits: A Focus on Medical Evidence Mass tort and class action lawsuits are essential legal mechanisms for addressing harm caused by corporate negligence, defective products, or environmental disasters. Though both involve groups of plaintiffs (the people bringing a case against another in a court of law), the way […]
Clear Medical Documentation: The Key to Successful Disability Claims

Clear Medical Documentation: The Key to Successful Disability Claims A comprehensive and well-organized set of medical documentation is vital for the success of any disability claim. These documents provide essential evidence demonstrating your adherence to specific medical criteria and clearly illustrate how your condition impacts your ability to work or carry out daily activities. Proving […]
Medical Evidence and VA Disability Claims

Many veterans face the frustrating experience of having their VA disability claims denied due to insufficient medical evidence. According to a 2024 document by the VA Pact Act, the Top 3 reasons for VA Claim denials on decisions on disability claims are: Not Incurred/Caused by Service; No Diagnosis; Not Established by Presumption. This means that, […]
Veteran Story – William Davis

William Davis: “I was chasing my dreams. Now I’m living them.” These days, it’s hard to believe that William Davis ever struggled with social interaction or even getting a good night’s sleep. His friendly demeanor comes across immediately and his positive attitude is infectious. It’s easy to think that he’s sported the same youthful energy […]
Temporary 100 VA Disability After Surgery
The United States Veterans Affairs (VA) department, which serves to honor our country’s veterans, plays an essential role in providing various crucial services, including VA disability benefits. These services, however, are sometimes put on a hold due to significant body changes such as undergoing surgeries. In such scenarios, the department offers temporary 100% disability benefits […]
The VA Rating For Surgery Scars
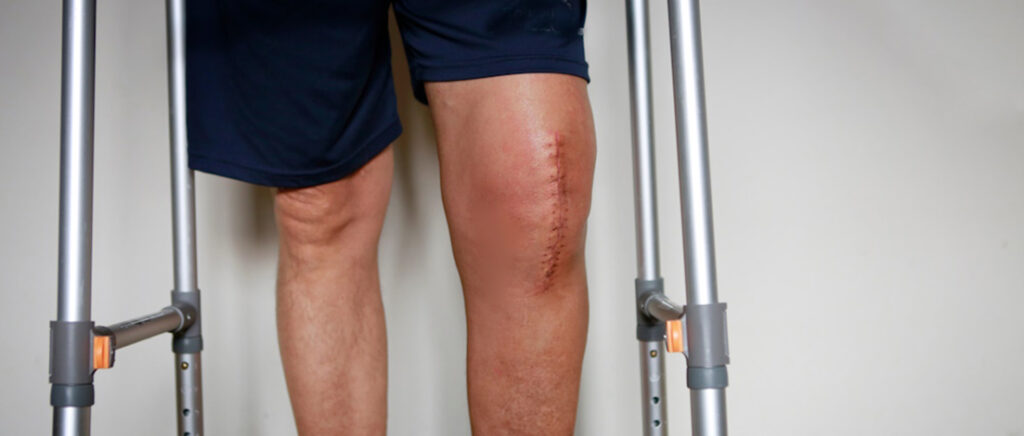
VA Rating: Surgery Scars and What Veterans Need to Know When it comes to determining a VA rating, surgery scars play a significant role in evaluating the impact of service-related injuries on a veteran’s life. The VA assesses these scars, often visible reminders of past sacrifices, to determine their effect on physical and psychological well-being. […]
Sleep Apnea VA Rating: A Comprehensive Guide for Veterans
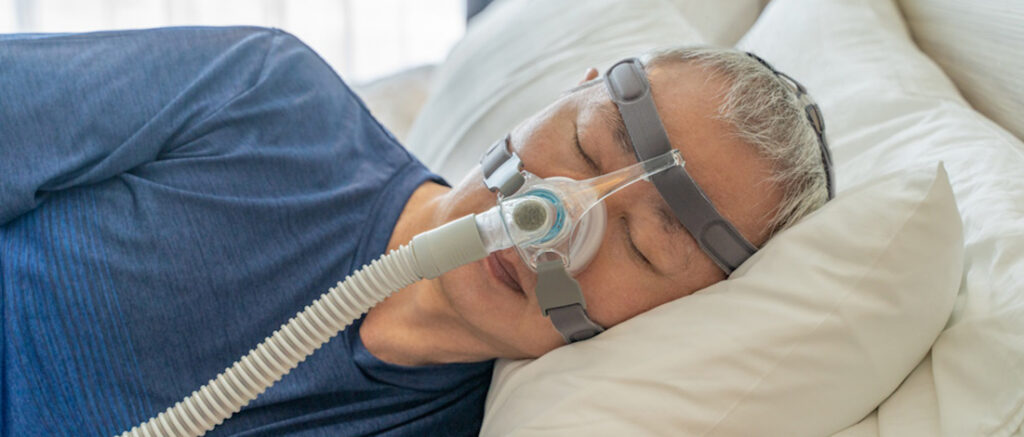
Sleep apnea, an easily overlooked but serious sleep disorder, has garnered significant attention in veteran circles due to its prevalence, impact on quality of life, and entanglement with the VA rating system. The Veterans Affairs (VA) rating system is crucial in determining the level of disability benefits a veteran receives and serves as a lifeline […]
Chronic Fatigue Syndrome VA Rating- Understanding Qualifying Conditions
Chronic fatigue syndrome, common among Gulf War veterans, is not only challenging to define but also difficult to diagnose. If you’re a veteran and diagnosed with chronic fatigue syndrome during or after your service, you might qualify for VA disability benefits. Unfortunately, defining, diagnosing, and proving chronic fatigue for VA disability is more difficult than […]


